Medicare fraud statistics show that billions of dollars are wasted every year due to scams and corruption. The damage to the entire healthcare system is irreparable, as that money could have been invested in a range of legal medical services.
Enormous expenses of fraudulent practices result in Medicare costs escalation. These scams also increase the risks of harming patients who undergo a range of unnecessary procedures.
Medicare fraud includes intentionally covering up the truth with the aim of obtaining illegitimate benefits. Paired with abuse, which involves practices that don’t adhere to authorized fiscal and medical practices to increase expenses, healthcare scams severely harm both the state and the federal medical system.
Latest Medicare Stats and Facts (Editor’s Picks)
- 18.1% of people in the US have Medicare
- In 2020, the Medicare improper payment rate was 6.27%
- Medicare spends almost $700 billion on its services
- Due to a single fraud, Medicare lost $2 billion
- In 2028, the US healthcare expenditures are projected to reach 6.2 trillion
- By investigating inaccurate payments, Medicare could have saved $367 million
- In 2028, Medicare expenditures are forecast to reach $1.5 trillion
Medicare Fraud Stats
According to federal law, frauds are recognized as criminal acts. They don’t harm only the organization they are targeted at. They may have a much wider impact and harm the entire industry or system, and therefore its direct and indirect beneficiaries. In terms of healthcare fraud, users and taxpayers bear the highest costs, according to healthcare fraud statistics.
1. The Medicare program spends nearly $700 billion on its services.
(Politifact)
The primary beneficiaries of Medicare services are people 65 years of age and older. The program also serves millions of disabled US citizens. Namely, almost $700 billion is spent every year on Medicare services, while the Medicare fraud estimates put the cost off fraudulent activities at around 7% of that sum. The program itself makes payments to 1 million entities.

2. 18.4% of Americans had some form of Medicare in 2020.
(Statista)
In 2019, over 18% of US residents were covered by its programs, accounting for almost 60 million people.
Medicare includes four major parts, with the first offering hospital coverage and the second medical coverage. The third provides an optional way to obtain Medicare benefits, whereas the fourth offers medicine prescription coverage. Medicare fraud stats suggest that all parts of the insurance scheme are vulnerable to scams and abuse, with roughly 3–4% of insurance claims being fraudulent.
3. Medicaid has an improper payment rate of 14.90%.
(CMS)
Inconsistencies in payments may not necessarily mean fraud or abuse, but do indicate a human error. The Medicare fraud rate shows that the program has the highest improper payment rate among its peers, at nearly 15%. In cash, this amounts to $57.36 billion.
Medicare FFS has an improper payment rate of 7.25% ($28.91 billion), Medicare Part B of 7.87% ($16.73 billion), and CHIP of 15.83% ($2.74 billion). Medicare Part D has the lowest rate of only 0.75% which amounts to $0.61 billion.
4. The rate of Medicare FFS improper payments was 6.27% in 2020.
(CMS)
That translated to almost $26 billion in improper payments. In 2019, the improper payment rate was 7.25%, leading to $28.91 billion in improper payments. In such cases, a health insurance fraud investigation process is required.
5. US doctors believe overtreatment is common, with 20.6% of procedures being obsolete.
(Pacific Prime)
Healthcare fraud and abuse statistics indicate that doctors deem more than a fifth of all prescribed procedures, tests, and medications unnecessary. Nearly 85% of doctors believe the main reason for overtreatment is a fear of being sued for malpractice. However, around 70% of physicians believe their colleagues are more likely to do unnecessary procedures when they can gain profit from it.

6. Healthcare fraud may result in 10-year imprisonment.
(Oberheiden P.C.)
According to the federal law on medical frauds, a common offense carries a prison sentence of up to 10 years. In the case that there was a bodily injury involved, the sentence increases to up to 20 years. Should the fraud result in death, life imprisonment is an option.
False claims typically result in criminal or civil penalties. The former requires hundreds of thousands of dollars to be paid, whereas the latter involves paying a fee of $21,000 per false claim.
How does fraud and abuse impact the costs of healthcare?
7. Medicare fraud costs insurers $50 billion annually.
(Politifact)
Scams are extremely expensive. An inconceivable amount of cash is wasted, without any alternative to rebound it. Medicare fraud costs are estimated at a whopping $50 billion a year. In other words, this is $1 billion per week spent.

8. The US lost $487 billion due to scams and human error.
(Gray Matter Analytics)
The Coalition Against Insurance Fraud estimates that medical frauds, as well as human error, cost America $487 billion annually. This figure makes up about 10% of the overall healthcare expenditure. In addition, the Medicaid error rate was about 9.8% with total spending of $300 billion in 2015. That’s a pretty huge amount of money lost to scams and human error.
9. Medicare programs lost $2 billion to just 1 fraud.
(Gray Matter Analytics)
Two years ago, 600 fraudsters (the majority of whom were healthcare workers) across 58 federal districts participated in a historical multi-agency scam. The scheme was focused on the distribution of opioids and other hazardous drugs. This Medicare fraud cost its crucial programs a colossal $2 billion.
10. Medicare could spare $367 million by checking improper payments.
(Health Payer Intelligence)
Medicare fraud waste and abuse statistics allege that 61% of Medicare payments for outpatient treatment claims were inadequately filed. Research showed that out of 300 sample claims, only 116 were filed correctly. Such an error cost the insurer almost $367 million.
11. Medicare spent $160.8 million on medications covered by hospices.
(Health Payer Intelligence)
The authorities discovered yet another instance of healthcare fraud and abuse with Medicare. Namely, Centers for Medicare and Medicaid Services paid over $160 million on medications for Medicare Advantage. The issue here is that hospices already cover those drugs.
12. In 2020, America spent $4.1 trillion on medical care.
(CMS)
That equated to $12,350 worth of costs per person. A great deal of the sum the US invests in health care is often used to compensate for health insurance claims. But, medicare fraud and abuse statistics suggest that there is a high number of fraudulent claims.
As false claims, frauds, and abuse may cost up to $300 million, one can’t help but conclude that such false claims are highly expensive, regardless of the fact they might make up only a small portion.
13. The US government spendings on healthcare will be $6.2 trillion in 2028.
(CMS, Tax Policy Center)
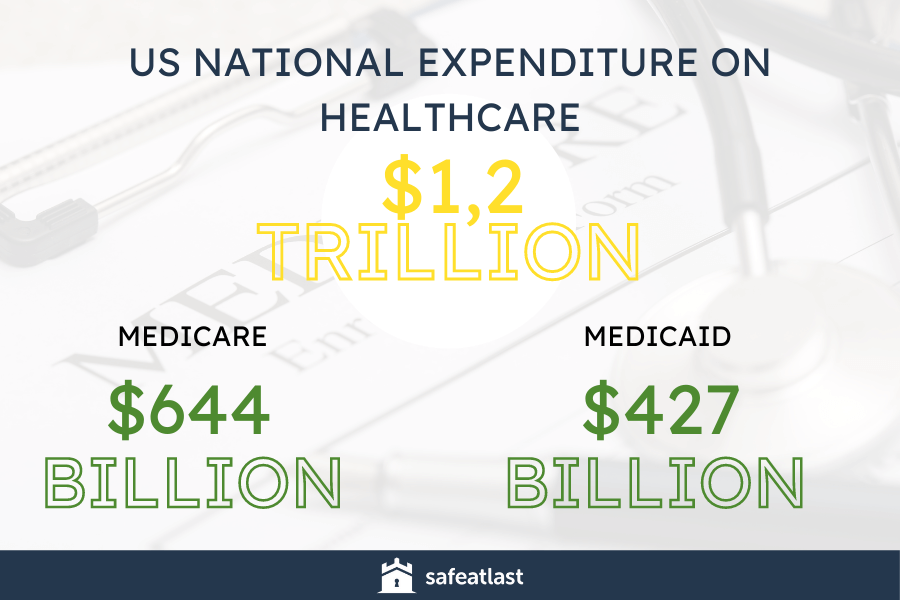
National expenditure on healthcare amounted to $1.2 trillion in 2019. Out of that amount, $644 billion and $427 billion were assigned to Medicare and Medicaid & the Children’s Health Insurance Program, respectively.
In 2028, the national spendings are expected to reach a whopping $6.2 trillion, so the cost of Medicare fraud shouldn’t be discounted.
14. Fraud and abuse comprise between 3% and 10% of total healthcare spendings.
(NHCAA)
The National Healthcare Anti-Fraud Association estimates that health care scams incur billions of dollars of losses every year, as much as 10% of annual healthcare spendings. In figures, this can equal to over $300 billion every year. This can lead to higher premiums, reduced benefits, and out-of-pocket costs for clients.
15. Around $1.4 billion was given back to Medicare Trust Funds.
(GAO)
Medical fraud statistics reveal that the Office of Inspector General at HHS and the US Department of Justice managed to return nearly $1.4 billion to Medicare Trust funds via fines, forfeits, and recoveries. These departments actively fight healthcare and insurance frauds and prosecute perpetrators.
16. Medicare costs are expected to rise to $1.5 trillion in 2028.
(GAO, CMS)
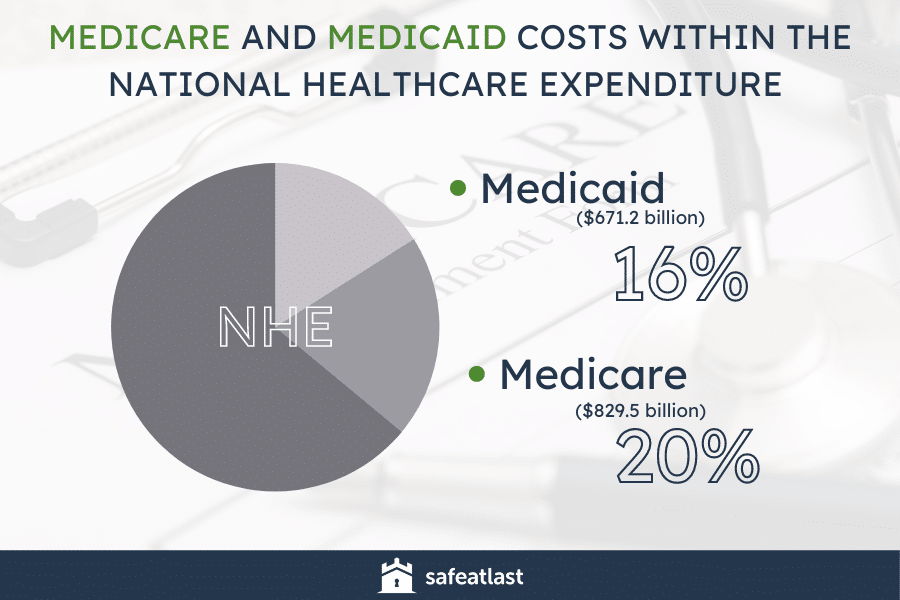
In 2020, Medicare expenditure amounted to $829.5 billion, which stands for 20% of the national healthcare expenditure (NHE). Medicaid accounted for 16% of the overall NHE, or $671.2 billion.
As for Medicare fraud trends, these expenditures are bound to reach $1.5 trillion by 2028, i.e., 5.1% of GDP and 21.9% of federal spendings.
The Bottom Line: How Much Fraud Is There in Medicare
Medicare covers around 60 million people in the US, which accounts for over 18% of the population. The program is funded by users’ premiums, payroll tax, and general revenues, so the Medicare fraud numbers are nothing to be scoffed at. Considering the fact that the US investments in healthcare increase annually — from $3.6 trillion in 2018 to an estimated $6.2 trillion in 2028 — it’s not surprising that the medical system is an easy target for fraud, waste, and abuse.
On a yearly basis, Medicare spends nearly $700 on its services. Taking that colossal amount into consideration, it doesn’t come as a surprise that it’s a favorite target for frauds and abuse. As Medicare fraud statistics unveil, it loses $50-$60 billion dollars every year to scams and false claims. What’s more, in only one multi-agency fraud, it lost $2 billion.
However, such frauds aren’t treated lightly. An array of law enforcement agencies collaborate with the FBI on investigating medical frauds. The punishments vary from a fee to a prison sentence, depending on the level of involvement in the final outcome.
People Also Ask
What are the common types of Medicare fraud?
There are numerous scams and frauds concerning Medicare that are wasting client and taxpayer money. Major categories of healthcare fraud and abuse include deeds such as:
– Submitting claims for services that patients never underwent or received
– Falsifying diagnoses and claims
– Offering free services, goods, or any other reimbursement to get others’ Medicare number
– Billing Medicare for equipment or supplies that are never received
– Using somebody else’s Medicare number or card
– Offering a patient a Medicare medication plan that is not approved
– Giving false information to a patient in order to sign them up for a Medicare plan
– Taking part in unlawful kickback or referrals
– Prescribing unneeded drugs
– Upcoding for pricey and unwarranted services
Who commits the most Medicare fraud?
Perpetrators may vary, from large corporations and organizations created just to commit fraud to patients and individual providers. However, the most frequent participants and offenders include medical providers who tend to submit claims for unnecessary or unprovided services, Medicare fraud and abuse statistics show.
Suppliers are also among frequent perpetrators, as they may choose to bill items or equipment they don’t provide. Companies, especially non-healthcare ones, may give unapproved plans or mislead prospective clients to join them. Lastly, beneficiaries can also commit fraud by allowing third-parties to use their Medicare card or giving their ID number for money or other incentives, Medical fraud stats indicate.
What is considered Medicare fraud?
A Medicare fraud happens when individuals intentionally deceive Medicare to get paid when they are not supposed to. Also, they may go in for a higher payment compared to the one they should receive. Anyone can participate in or commit a fraud — physicians or any other medical staff, suppliers, and Medicare clients. It’s essential to note that such fraud is illegal and will be prosecuted. Additionally, it’s important to note the high cost of Medicare fraud and abuse, which is a burden on taxpayers.
Who investigates Medicare fraud?
The FBI is the central law enforcement agency responsible for exposing any kind of healthcare fraud. It has jurisdiction over both federal and private insurance programs. Medical fraud and abuse are regarded as a top priority within the Complex Financial Crime Program. Therefore, every of the Bureau’s offices employs staff whose assignment is to investigate medical fraud and abuse cases, so as to lower Medicare fraud rates.
The FBI collaborating with other agencies as well, such as the Office of Inspector General at Health and Human Services (HHS OIG), the FDA and the DEA, the Defense Criminal Investigative Service (DCIS), and the Internal Revenue Service-Criminal Investigation (IRS-CI). Medicaid Fraud Control Units from other states and state and local law enforcement agencies are also included.
What are the penalties for Medicare fraud?
Federal agencies may charge civil or criminal penalties. In general, civil cases include unintentional fraud allegations. On the other hand, criminal cases demand evidence that the perpetrator intentionally filed a fraudulent claim for Medicare compensation.
Civil penalties involve paying a fine amounting to $21,000 per a fraudulent claim, reimbursement for overbilled amounts, and treble damages. Criminal cases require paying a fine amounting to hundreds of thousands of dollars, and carry a prison sentence of between 5 and 20 years, and can sometimes even include a lifetime prison sentence.
How much Medicare fraud is present in the United States?
Taking into account the money lost to fraud and abuse (over $50 million a year), as well as millions lost to improper payments, while the exact Medicare fraud amount is hard to determine, it could be concluded that Medicare fraud is relatively frequent. Not all scam instances are intentional, though — some are committed unknowingly.
What is the difference between Medicare fraud and abuse?
Medicare fraud involves intentional and calculated deception or misstating of services an individual is aware of are false. Such a case may result in additional and illegal remuneration or payments to a practice.
Medicare abuse is regarded as a lesser offense that happens when medical offices do not adhere to correct coding and billing regulations and guidelines. Generally, abuse refers to matters or practices that don’t comply with established healthcare, business, or fiscal procedures.
According to Medicare fraud statistics, fraud can also involve identity theft in some cases, whereas abuse generally does not.

Leave a Reply
You must be logged in to post a comment.